Psoriasis treatment: clear options and how to pick what works
Psoriasis can be stubborn, but you don’t have to guess your way through treatment. If patches are small and mild, simple fixes often work. If they cover large areas, hit joints, or won't budge, stronger options are available. This quick guide helps you understand the main choices, what they do, and what to ask your doctor.
Topical treatments and basic care
Start with the basics: moisturize, gentle cleansing, and steroid creams when needed. Thick emollients soothe dryness and cut scaling. Over-the-counter options include urea, salicylic acid, and coal tar products — these soften skin and let other medicines work better.
Topical corticosteroids reduce inflammation fast. Use the lowest strength that works and follow your doctor’s schedule to avoid thinning skin. Vitamin D analogues (calcipotriene) help slow skin cell growth and pair well with steroids. For sensitive areas like the face or groin, milder formulations are safer.
Light therapy, pills, and injections
Phototherapy uses controlled UVB light to calm the immune response in skin. It works well for widespread psoriasis and is a good option if creams don’t cut it. Clinics offer narrow-band UVB; some people use home units under doctor guidance. PUVA (a drug plus UVA) is effective but has more side effects, so doctors reserve it for tougher cases.
Oral and injected systemic drugs treat moderate-to-severe disease or psoriatic arthritis. Traditional choices include methotrexate, cyclosporine, and acitretin. They’re powerful but need regular blood tests and monitoring.
Biologics target specific immune signals that drive psoriasis. Drugs like adalimumab, secukinumab, and others often clear skin dramatically when other treatments fail. Biologics require screening (TB, hepatitis) and a plan for vaccines and infection monitoring. Talk with your specialist about safety, how fast they work, and long-term plans.
Side effects matter. Every systemic drug carries risks—liver tests, blood counts, blood pressure checks, and watching for infections are common steps. Your doctor should explain monitoring and what to report immediately.
Small lifestyle moves help too. Keep skin moist, avoid smoking, limit alcohol, manage weight, and find ways to lower stress. Losing even a little weight or cutting back on booze can reduce flare frequency for many people.
When to see a dermatologist? If psoriasis affects your face, hands, feet, nails, or genitals, or covers a large area or limits daily life, get specialist care. Also see a doctor if you have joint pain—psoriatic arthritis needs early treatment to avoid damage.
Questions to ask: What are the realistic results and timeline? What side effects should I expect? How often will I need tests? Can I combine treatments safely? A quick conversation can save weeks of trial-and-error.
Want deeper reads on specific drugs or alternatives? Check our site for guides on biologics, steroid alternatives, and practical buying tips. Treating psoriasis is a process, but with the right plan you can get clear, comfortable skin—often sooner than you expect.
Learn the latest psoriasis treatment options for plaque, guttate, and systemic forms in 2025. Discover how biologics, oral drugs, and targeted therapies are changing outcomes - with real data on efficacy, cost, and patient experiences.
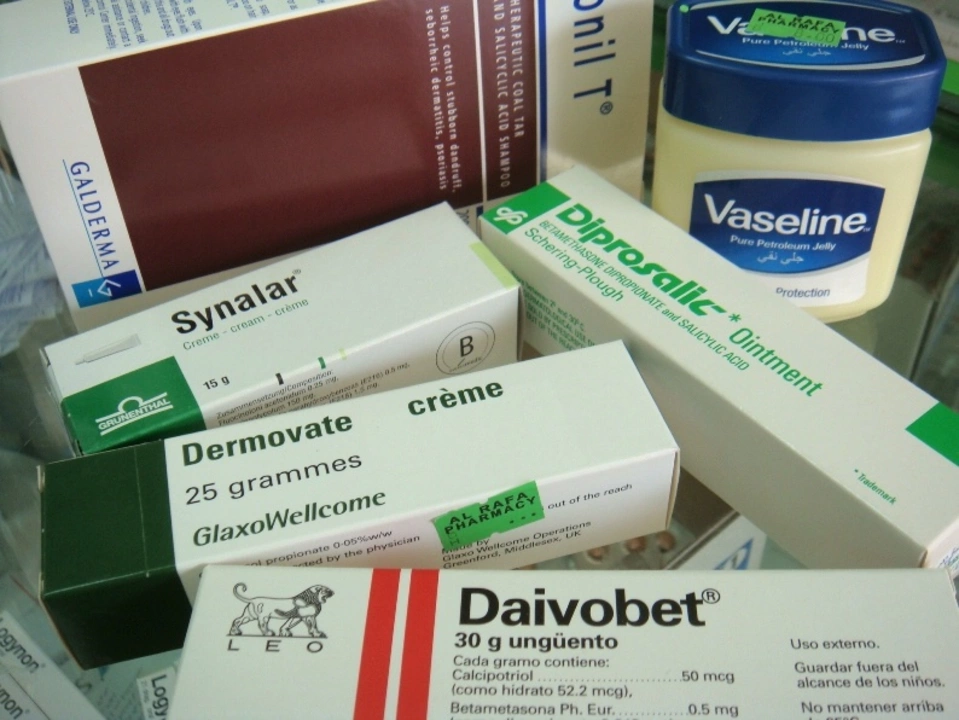
In my recent research, I discovered an interesting connection between Calcipotriol and Vitamin D. Calcipotriol, a synthetic derivative of Vitamin D, is commonly used to treat psoriasis by promoting normal skin cell growth. This link highlights the importance of Vitamin D in maintaining healthy skin and preventing skin conditions. It's fascinating to see how a compound derived from a vitamin we often associate with bone health plays such a crucial role in skincare. So, next time you're out in the sun, remember that you're not just strengthening your bones, but also taking care of your skin!