Allergies: Causes, Quick Relief, and Long-Term Control
Allergies can ruin a day fast — watery eyes, sneezing, itchy throat, or a tight chest. About one in five people deal with allergic symptoms every year. The good news: most reactions are manageable with straightforward steps you can start today. This page gives clear, practical advice so you spend less time guessing and more time feeling normal.
What causes allergies and common signs
An allergy happens when your immune system overreacts to something harmless: pollen, dust mites, pet dander, mold, or certain foods and medicines. Classic signs are sneezing, runny or blocked nose, itchy or red eyes, skin rashes or hives, and sometimes wheeze or shortness of breath. Symptoms can be seasonal (pollen) or year-round (dust mites, pets).
Not every sniffle is an allergy. A cold usually comes with fever and thick yellow mucus. If your symptoms flare every spring or every time you hug the cat, that points to allergies.
Quick relief you can try today
Need fast help? Over-the-counter antihistamines work well for most people: cetirizine, loratadine, or fexofenadine cause little drowsiness and ease sneezing and itching. For nasal congestion, a short course of a decongestant or a steroid nasal spray (like fluticasone) can be more effective. Use nasal sprays daily for best effect — they take a few days to peak, but they really reduce swelling.
Eye drops for allergic eyes and saline nasal irrigation are inexpensive and safe. If you have asthma or severe reactions, follow your action plan and keep rescue inhalers or epinephrine (if prescribed) on hand. Ask a pharmacist if you’re unsure which OTC option fits your situation.
Avoid risky mixes: some antihistamines can make you drowsy, and combining several cold meds raises side-effect risk. Pregnant or breastfeeding? Check with a clinician before starting any medicine.
Long-term control matters more than quick fixes. Reducing exposure stops symptoms before they start. Use dust-mite covers, wash bedding hot weekly, run HEPA or true-filter air purifiers, keep indoor humidity under 50% to limit mold, and keep pets out of bedrooms. For pollen season, close windows during high-count days and shower after being outside.
If medicines don’t control your symptoms, ask about allergy testing and immunotherapy. Allergy shots or tablets can reduce sensitivity over time and lower the need for daily meds. They’re not instant, but they can change how your immune system reacts.
When should you see a doctor? Get urgent help for breathing trouble, throat swelling, fainting, or a rapid spread of hives. Book an allergy or respiratory specialist if symptoms last despite treatment, affect sleep or work, or if you need frequent steroid courses. A quick evaluation can often make life much easier.
Small changes add up. Track triggers in a notebook for two weeks, try one change at a time, and keep a simple plan: reduce exposure, use safe OTC meds, and see a specialist when needed. That approach solves most allergy problems without stress or guesswork.
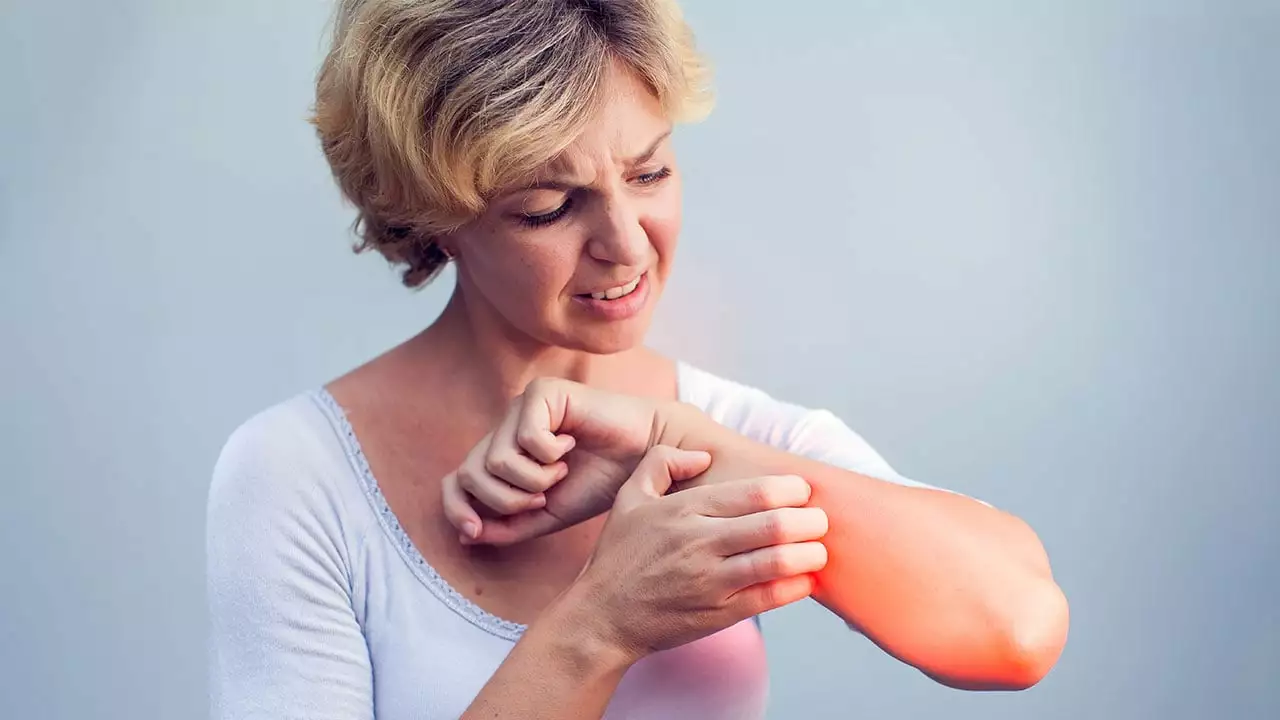
I recently explored the fascinating connection between skin irritations and food sensitivities. It turns out that certain foods can cause or exacerbate skin issues like eczema, acne, and rashes. This happens because our body reacts to these trigger foods by releasing inflammatory chemicals, which can manifest as skin problems. Identifying and eliminating these foods from our diet can significantly improve our skin health. So, it's definitely worth paying attention to what we eat and how it affects our skin.