Chloasma (Melasma): What It Is and What You Can Do Today
Chloasma—also called melasma—shows up as brown or gray patches on your face. It’s common during pregnancy and when hormones shift, but sun exposure, certain meds, and heat can trigger it too. If you’ve noticed patchy dark areas on your cheeks, forehead, or upper lip, this guide gives clear, doable steps to reduce their look and stop them getting worse.
What causes chloasma?
Hormones are the main driver. Pregnant people often get it (up to about half do). Birth control and hormone therapy can also spark it. Sun and UVA/visible light make pigment cells overproduce melanin, so UV protection is crucial. Certain skincare or hair removal that irritates skin can worsen it through inflammation. Genetics play a role—some skin types are just more likely to get melasma.
Practical treatment plan you can start now
Start with sun protection. Use a broad-spectrum sunscreen with at least SPF 50 every morning. Physical filters (zinc oxide, titanium dioxide) work well. Reapply every two hours if you’re outdoors and wear a wide-brim hat and sunglasses. Sunscreen reduces new darkening and makes other treatments work better.
Gentle daily care: use a mild cleanser and avoid harsh scrubs or frequent waxing near patches. Heat can worsen melasma, so avoid hot-stone facials and excessive steam.
Topical options: azelaic acid (10–20%), kojic acid, and topical tranexamic acid can help and are safer during pregnancy than many other options—still check with your provider. Hydroquinone (2–4%) is the most studied pigment reducer and often works faster, but use it under a dermatologist’s guidance and avoid long-term unsupervised use. Tretinoin speeds cell turnover and enhances results but can irritate; combine carefully and use at night.
Procedures: chemical peels, microneedling, and certain laser treatments can improve melasma, but they carry risk—especially for darker skin tones, where post-inflammatory darkening is possible. Only get these from an experienced dermatologist who knows how melasma behaves.
Oral options: low-dose oral tranexamic acid is used off-label for stubborn melasma and can work well for some people. It requires a doctor’s supervision because of potential blood-clot risks and other side effects.
Realistic timeline: expect gradual improvement over weeks to months. Most topical regimens need at least 8–12 weeks to show clear change, and maintenance (sun protection, ongoing topical use) is often needed to prevent return.
Quick safety tips: patch-test any new product, avoid unregulated skin-bleaching creams (they may contain mercury or unsafe steroids), and talk to a dermatologist before trying aggressive treatments or combining prescription products. If you’re pregnant or breastfeeding, consult your provider before starting most prescription treatments.
Want help picking a safe plan? A short visit with a dermatologist can give you a tailored approach—one that balances speed, safety, and keeping your skin healthy long term.
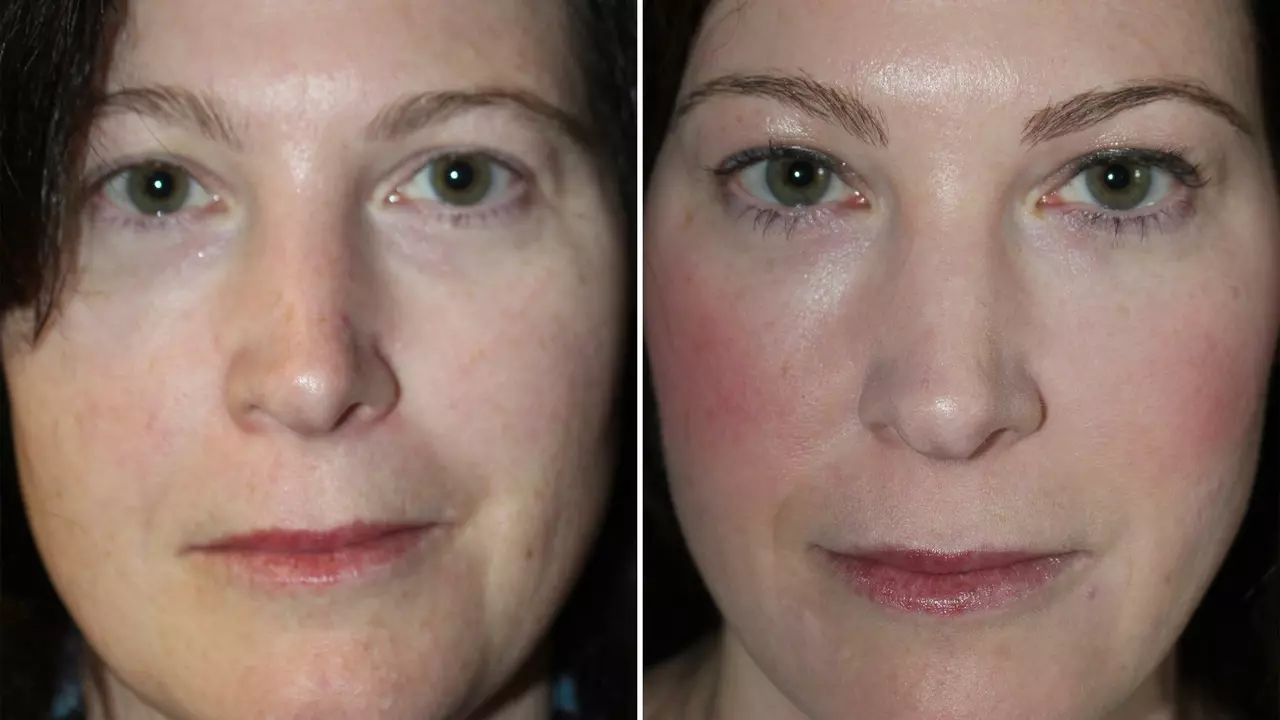
In exploring the effectiveness of chemical peels for chloasma, I've discovered numerous benefits. Chemical peels have been found to reduce the appearance of these dark patches, often caused by hormonal changes or sun exposure. They essentially exfoliate the skin, removing the damaged outer layers and promoting new, healthier skin growth. However, their effectiveness can depend on various factors, including the type and depth of peel, so it's crucial to consult with a professional. Overall, they offer a promising treatment option for chloasma sufferers.