Drug-Induced Lupus Recovery Calculator
How Your Medication Affects Recovery
Drug-induced lupus (DIL) often resolves completely when the triggering medication is stopped. Recovery times vary depending on the drug and individual factors.
Your Expected Recovery Timeline
Recovery Estimate
Medication Risk Profile
Symptom Improvement Timeline
Symptoms typically begin to fade
Most patients see significant improvement
95% of patients achieve full recovery
Important Notes
- Discontinuing the medication is the most important step for recovery
- If symptoms are severe (like chest pain), medical treatment may be needed
- Never stop prescribed medications without consulting your doctor
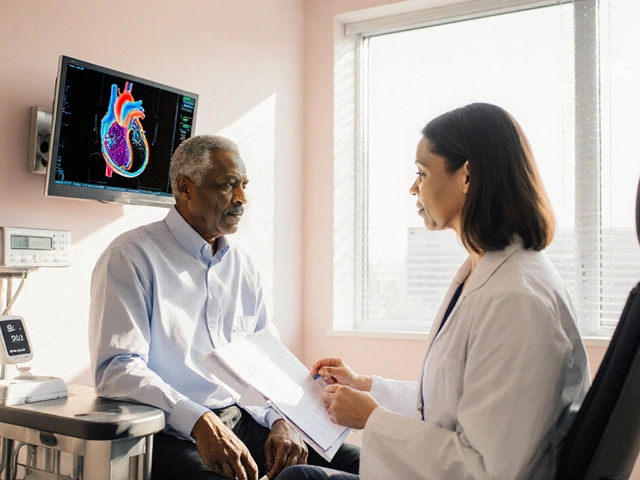
Most people think lupus is a lifelong autoimmune disease you’re born with. But what if your body suddenly started attacking itself-not because of genetics, but because of a pill you took for high blood pressure, acne, or heart rhythm? That’s drug-induced lupus (DIL), and it’s more common than you think. Unlike classic lupus, DIL isn’t permanent. It doesn’t usually damage kidneys or the brain. And here’s the best part: drug-induced lupus often goes away completely once you stop the medicine causing it.
What Actually Triggers Drug-Induced Lupus?
Drug-induced lupus isn’t caused by one mysterious substance. It’s linked to about 50 different medications, but only a few are big players. Hydralazine (for high blood pressure) and procainamide (for irregular heartbeat) are the classic culprits. Up to 30% of people on long-term procainamide develop DIL. Hydralazine isn’t far behind-5% to 10% of users over time. These drugs have been around for decades, but their link to lupus-like symptoms wasn’t fully understood until the 1950s.
Today, newer drugs are rising in the ranks. TNF-alpha inhibitors-used for rheumatoid arthritis, Crohn’s disease, and psoriasis-are now responsible for 12% to 15% of new DIL cases. Minocycline (an acne antibiotic) and immune checkpoint inhibitors (used in cancer therapy) are also on the list. The risk isn’t huge for these newer drugs-usually 1% to 3%-but because they’re used so widely, the total number of cases is growing.
It’s not just about the drug. Your genes matter too. If your body is a slow acetylator (a genetic trait that affects how fast you break down certain drugs), your risk of developing DIL from hydralazine jumps nearly five times higher. And if you carry the HLA-DR4 gene, your chances go up over threefold. That’s why some European guidelines now recommend genetic testing before starting hydralazine.
How Do You Know It’s DIL and Not Regular Lupus?
The symptoms of drug-induced lupus look a lot like systemic lupus erythematosus (SLE). Joint pain. Fatigue. Fever. Muscle aches. But there are key differences.
- Joint and muscle pain: Affects 75% to 85% of DIL patients. Often symmetric, like rheumatoid arthritis.
- Fatigue and fever: Nearly everyone feels tired. Fever shows up in more than half.
- Serositis: Inflammation around the heart (pericarditis) or lungs (pleuritis) happens in 25% to 35% of cases. This is more common in DIL than in classic lupus.
- Skin rash: Only 10% to 15% get the classic butterfly malar rash. Photosensitivity (sun sensitivity) is also less common than in SLE.
- Organ damage: Kidney disease? Less than 5% of DIL cases. Brain or nervous system problems? Under 3%. In regular lupus, those numbers are 30% to 50% and 20% to 30% respectively.
That’s the first clue: if you’re over 50, and you’ve got lupus-like symptoms without kidney or brain involvement, DIL is far more likely than SLE. SLE usually hits younger women. DIL? It’s equal in men and women-and mostly seen in older adults.
Testing for Drug-Induced Lupus
There’s no single test that confirms DIL. Diagnosis is a puzzle made of three pieces: your medication history, your symptoms, and your blood results.
First, doctors look at what drugs you’ve been taking. If you started a new medication 3 to 6 months ago (sometimes as early as 3 weeks, or as late as 2 years), that’s a red flag. The timing matters. DIL doesn’t show up overnight.
Next, blood tests. Over 95% of DIL patients test positive for antinuclear antibodies (ANA). But that’s not specific-it’s also positive in SLE, rheumatoid arthritis, even some healthy people.
The real game-changer? Anti-histone antibodies. About 75% to 90% of DIL patients have them. That’s rare in regular lupus-only 50% to 70% of SLE patients do. If you’re ANA-positive and anti-histone-positive, especially if you’re on hydralazine or procainamide, DIL is very likely.
Another key test: anti-dsDNA. This antibody is present in 60% to 70% of SLE patients. In DIL? Less than 10%. So if your anti-dsDNA is negative and anti-histone is positive, it points strongly to DIL.
Other markers like ESR (erythrocyte sedimentation rate) and CRP (C-reactive protein) are often elevated, showing inflammation-but they don’t tell you the cause.
What Happens When You Stop the Drug?
This is where DIL is different from almost every other autoimmune disease: it’s reversible.
Once you stop the triggering medication, symptoms begin to fade. Most people see improvement within 2 to 4 weeks. Eighty percent notice major relief by the end of the first month. By 12 weeks, 95% of patients are significantly better.
Some people need help along the way. Mild symptoms like joint pain and fatigue often respond to over-the-counter NSAIDs like ibuprofen. About 60% to 70% of patients get relief this way.
If symptoms are more severe-say, chest pain from pericarditis or trouble breathing from pleuritis-doctors may prescribe a short course of low-dose corticosteroids. Prednisone at 5 to 10 mg daily for 4 to 8 weeks usually clears things up. Rarely, you might need stronger immunosuppressants like azathioprine or methotrexate, but that’s uncommon.
And here’s the hopeful part: once symptoms disappear, most people don’t need to take any long-term medication. No lifelong steroids. No daily immunosuppressants. Just stop the drug, let your immune system reset, and you’re back to normal.
What If You Need the Original Medication?
Some people can’t just stop their meds. A person with a dangerous heart rhythm might need procainamide. Someone with severe hypertension might rely on hydralazine.
In those cases, doctors switch to safer alternatives. For heart rhythm, amiodarone is a good option-it carries only a 0.1% to 0.3% risk of DIL. For high blood pressure, ACE inhibitors or calcium channel blockers are preferred over hydralazine.
Switching isn’t always easy. But the risk of staying on the bad drug far outweighs the inconvenience. One patient on a lupus forum shared: “I was on hydralazine for 18 months. My joints hurt so bad I couldn’t open jars. My doctor switched me to lisinopril. Within three weeks, the pain was gone. I didn’t even need steroids.”

Why Do People Get Misdiagnosed?
Up to 25% of DIL cases are first mistaken for systemic lupus. Why? Because the symptoms overlap. Many doctors don’t think to ask about medications. Or they assume lupus = lifelong.
Patients often get misdiagnosed with fibromyalgia or chronic fatigue syndrome. One 2022 survey found the average time from first symptom to correct DIL diagnosis was 4.7 months. That’s nearly five months of unnecessary pain, tests, and anxiety.
And here’s the scary part: if you’re wrongly diagnosed with SLE, you might be put on long-term steroids or immunosuppressants you don’t need. That means higher risk of infections, bone loss, weight gain, and diabetes-all avoidable if DIL is caught early.
What’s Changing in DIL Diagnosis Today?
Things are getting better. In March 2023, the American College of Rheumatology released new diagnostic criteria for DIL. It now includes specific timeframes for drug exposure and symptom resolution. This helps doctors spot it faster.
Research is also moving toward prediction. Scientists are studying microRNA patterns in the blood to find early warning signs before symptoms even appear. One study is even testing “histone decoy” molecules that could block the immune reaction without stopping the drug-potentially letting people stay on life-saving meds without getting lupus.
With more people on biologics and immune-modulating drugs, DIL cases are expected to rise by 15% to 20% by 2030. But better awareness and faster testing mean we’ll catch more cases before they cause lasting damage.
What Should You Do If You Suspect DIL?
If you’re on one of the high-risk drugs-hydralazine, procainamide, minocycline, TNF inhibitors-and you’ve developed new joint pain, fatigue, or chest discomfort:
- Write down every medication you’ve taken in the last 2 years, including doses and start dates.
- See your doctor. Ask: “Could this be drug-induced lupus?”
- Request ANA and anti-histone antibody tests.
- If anti-dsDNA is negative and you’re over 50, DIL is likely.
- Don’t stop your medication without medical supervision. Some drugs need to be tapered.
- Track your symptoms. Improvement within weeks of stopping the drug confirms DIL.
Remember: this isn’t your fault. It’s not a weak immune system. It’s a reaction between a drug and your body’s chemistry. And it’s fixable.
Can drug-induced lupus come back after stopping the medication?
No, not if you avoid the triggering drug. Once you stop the medication and your symptoms resolve, DIL doesn’t return. Unlike systemic lupus, there’s no chronic immune memory. The only exception is if you restart the same drug-then symptoms can reappear within days or weeks. That’s why doctors strongly advise against re-exposure.
Is drug-induced lupus dangerous?
It’s rarely life-threatening. Most cases involve joint pain, fatigue, and mild inflammation around the heart or lungs. These are uncomfortable but not fatal. Major organ damage like kidney failure or brain inflammation is extremely rare in DIL. The real danger is misdiagnosis-being treated for chronic lupus with long-term steroids when you don’t need them.
How long does it take to recover from drug-induced lupus?
Most people feel better within 2 to 4 weeks after stopping the drug. About 80% show major improvement by the end of the first month. Nearly all (95%) recover fully within 12 weeks. Some with more severe symptoms may need a short course of steroids, which usually clears things up in 4 to 8 weeks.
Can I get drug-induced lupus from over-the-counter drugs?
Very rarely. Almost all reported cases come from prescription drugs, especially those that affect the immune system or are metabolized slowly. There’s no solid evidence linking common OTC painkillers, cold medicines, or supplements to DIL. The main culprits are long-term prescription medications like hydralazine, procainamide, and certain biologics.
Are there any tests to predict if I’m at risk before taking a drug?
Yes, for some drugs. For hydralazine, genetic testing for NAT2 slow acetylator status can identify people at 4.7 times higher risk. This is now recommended in some European countries before prescribing hydralazine. For other drugs, no routine test exists yet-but researchers are working on blood-based biomarkers that could predict risk before symptoms start.