Drug Clearance: How Your Body Processes Medications and Why It Matters
When you take a pill, your body doesn’t just hold onto it forever. Drug clearance, the rate at which a medication is removed from the bloodstream by the liver, kidneys, and other organs. Also known as elimination rate, it determines how long a drug stays active and how often you need to take it. If clearance is too fast, the medicine won’t work long enough. Too slow, and it builds up to dangerous levels. This isn’t just theory—it’s why your doctor adjusts your dose if you have kidney disease, liver problems, or take other meds.
Drug clearance ties directly to pharmacokinetics, how your body absorbs, distributes, metabolizes, and excretes drugs. It’s not the same as drug metabolism, the chemical breakdown of a drug, mostly in the liver, but metabolism is a big part of it. Think of clearance as the total exit plan: metabolism breaks the drug down, kidneys flush out the pieces, and sometimes the lungs or sweat help too. If you’re on a statin, an antibiotic, or even a sleep aid, your clearance rate affects whether it works, causes side effects, or interacts with something else you’re taking. That’s why bioequivalence, the measure that proves a generic drug behaves like the brand-name version in your body relies so heavily on clearance data. Two pills might look identical, but if one clears faster, it won’t work the same.
And it’s not just about the drug itself. Age, genetics, diet, and other medications change how fast clearance happens. A 70-year-old might clear a drug half as fast as a 30-year-old. Some people have liver enzymes that break down drugs too quickly—making standard doses useless. Others hold onto drugs like a sponge, risking overdose. That’s why drug interactions, when one drug changes how another is cleared are so dangerous. Grapefruit juice, for example, can block liver enzymes and slow clearance of certain statins to toxic levels. Antibiotics can do the same to blood thinners. These aren’t rare edge cases—they’re everyday risks you need to know about.
What you’ll find here are real-world guides that connect the dots between how drugs move through your body and how that affects your health. From understanding why your pharmacist asks about every supplement you take, to how partial AUC testing ensures generics work right, to why some meds need careful switching when side effects hit—this collection breaks down the science into what actually matters for you. No jargon. No fluff. Just clear answers to the questions you didn’t know to ask.
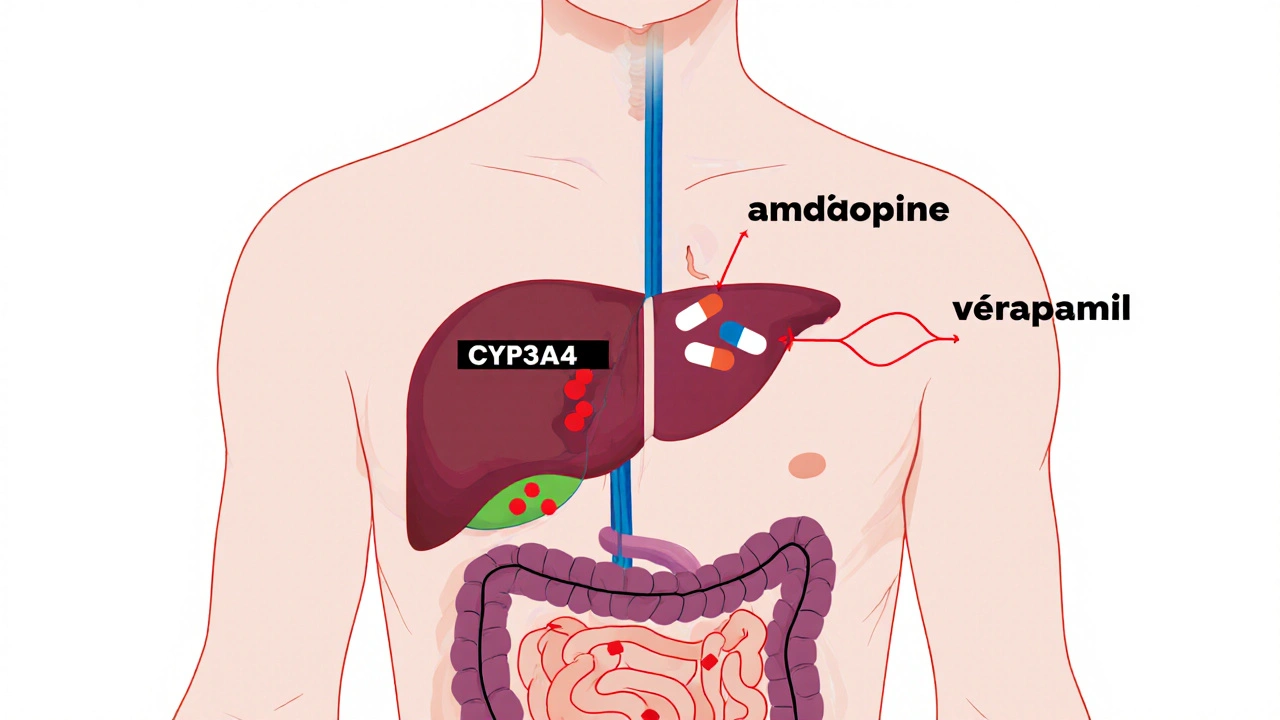
Calcium channel blockers are widely used for high blood pressure and heart conditions, but their safety depends heavily on how your body metabolizes them. Learn which ones are safest, which drugs and foods to avoid, and how to prevent dangerous interactions.






