Verapamil: What It Is, How It Works, and What Alternatives You Should Know
When your doctor prescribes verapamil, a calcium channel blocker used to treat high blood pressure and abnormal heart rhythms. Also known as a calcium channel blocker, it works by relaxing blood vessels and slowing down the heart’s electrical signals to reduce strain on your heart. Unlike some other heart meds, verapamil doesn’t just lower blood pressure—it also helps control fast or irregular heartbeats, making it a go-to for people with atrial fibrillation or angina.
It’s part of a group of drugs called calcium channel blockers, which also includes nifedipine, another common blood pressure medication that works faster but has a shorter effect, and diltiazem, a similar drug often used for heart rhythm issues. While nifedipine is great for quick relief of chest pain, verapamil is better for long-term rhythm control. Diltiazem sits in the middle—slower than nifedipine but less likely to cause swelling in the legs than verapamil. Each has trade-offs: verapamil can slow your heart too much if you’re not monitored, while nifedipine might cause headaches or flushing. Your body’s response matters more than the brand name.
If you’ve been on verapamil and noticed your heart feels slower, your legs are puffy, or you’re more tired than usual, you’re not alone. These are common side effects, but they don’t mean you need to quit. Often, a small dose change or switching to diltiazem fixes it. Some people switch to amlodipine, a longer-acting calcium blocker with fewer heart-rate side effects because it’s gentler on the rhythm. But if your main issue is an irregular heartbeat, not just high pressure, verapamil still holds its ground. It’s not the newest drug, but it’s one of the most studied—and for good reason.
What you’ll find below are real-world guides from people who’ve lived with these meds. You’ll read about how verapamil compares to other calcium channel blockers like nifedipine, what to do when side effects hit, how to tell if your heart rhythm is improving, and when it’s time to consider a switch. There’s also advice on monitoring your pulse, recognizing dangerous interactions, and what to ask your pharmacist when refilling your script. No fluff. No theory. Just what works—and what doesn’t—based on actual patient experiences and clinical insights.
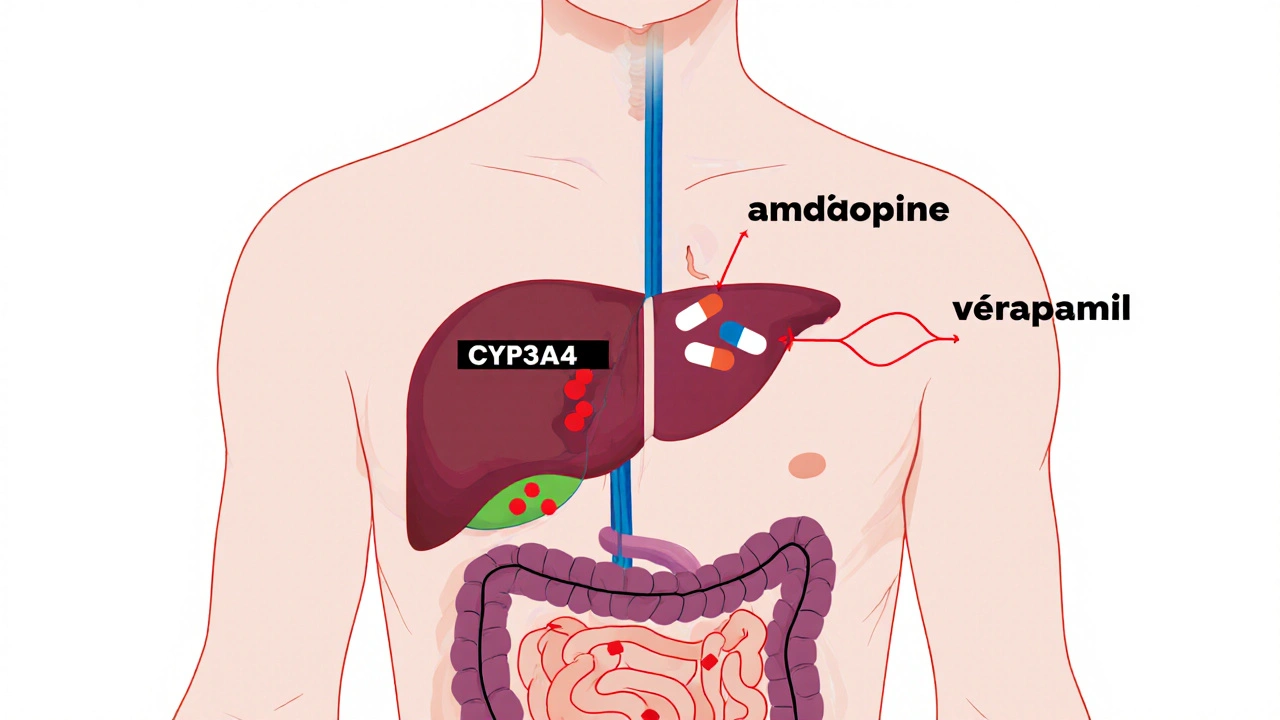
Calcium channel blockers are widely used for high blood pressure and heart conditions, but their safety depends heavily on how your body metabolizes them. Learn which ones are safest, which drugs and foods to avoid, and how to prevent dangerous interactions.