When you get a cut, scrape, or burn, your body starts healing right away-but how you care for it makes all the difference. Poor wound care doesn’t just slow things down; it can lead to infection, longer recovery, and scars that last for years. The good news? Simple, consistent steps can cut healing time by nearly half and reduce scarring by up to 70%. You don’t need fancy tools or expensive products. Just the right technique-and knowing what wound cleaning to avoid.
Step 1: Clean the Wound Properly
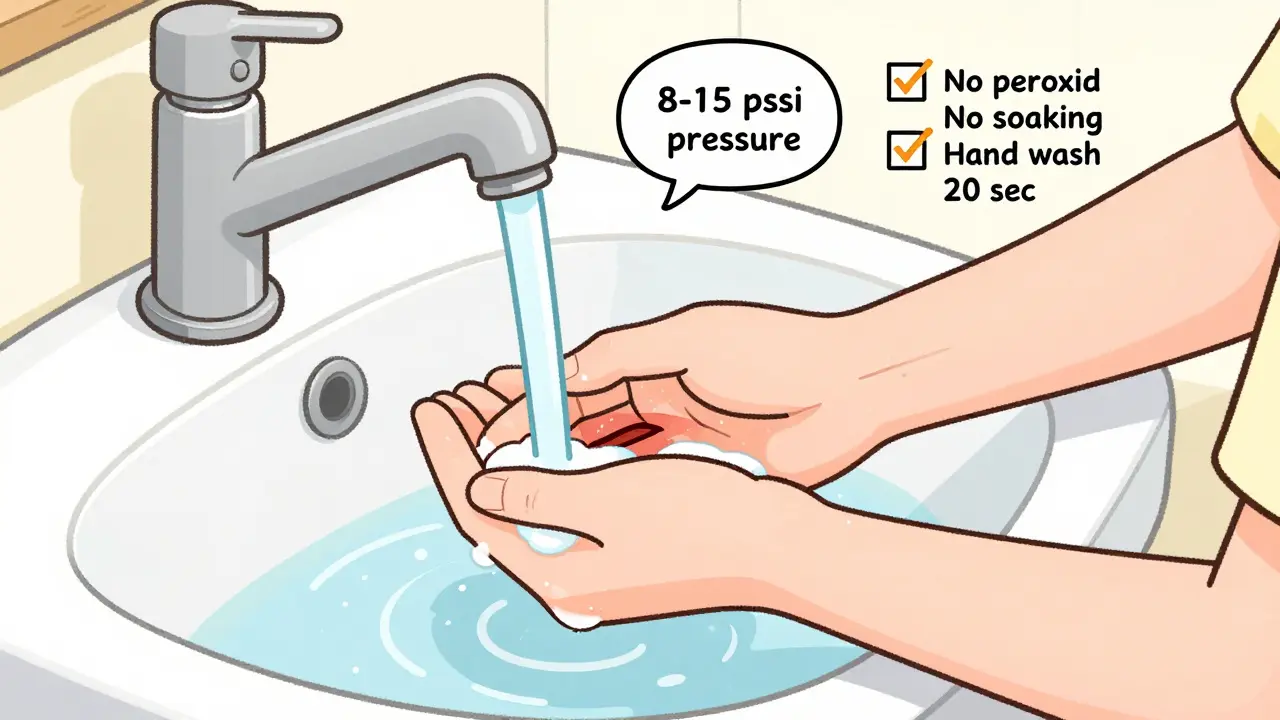
First thing: stop using hydrogen peroxide or rubbing alcohol. These might feel like they’re doing something, but they’re actually killing healthy tissue. Studies show they can delay healing by up to 50%. Instead, rinse the wound under cool running water for 5 to 10 minutes. The pressure of running water-about 8 to 15 psi-is enough to flush out dirt and bacteria without tearing delicate new skin. Don’t soak it in a bowl. Stationary water doesn’t move debris out; it just sits there.
Use mild soap on the skin around the wound, not inside it. Gently wash the area, then rinse again. If there’s visible grit or debris, use clean tweezers (sterilized with alcohol first) to remove it. Don’t dig. Don’t poke. If you can’t get it out, leave it. Let a professional handle it.
Hand hygiene matters too. Wash your hands with soap and water for at least 20 seconds-or use hand sanitizer with at least 60% alcohol-before and after touching the wound. This simple step cuts infection risk by 40%, according to the CDC.
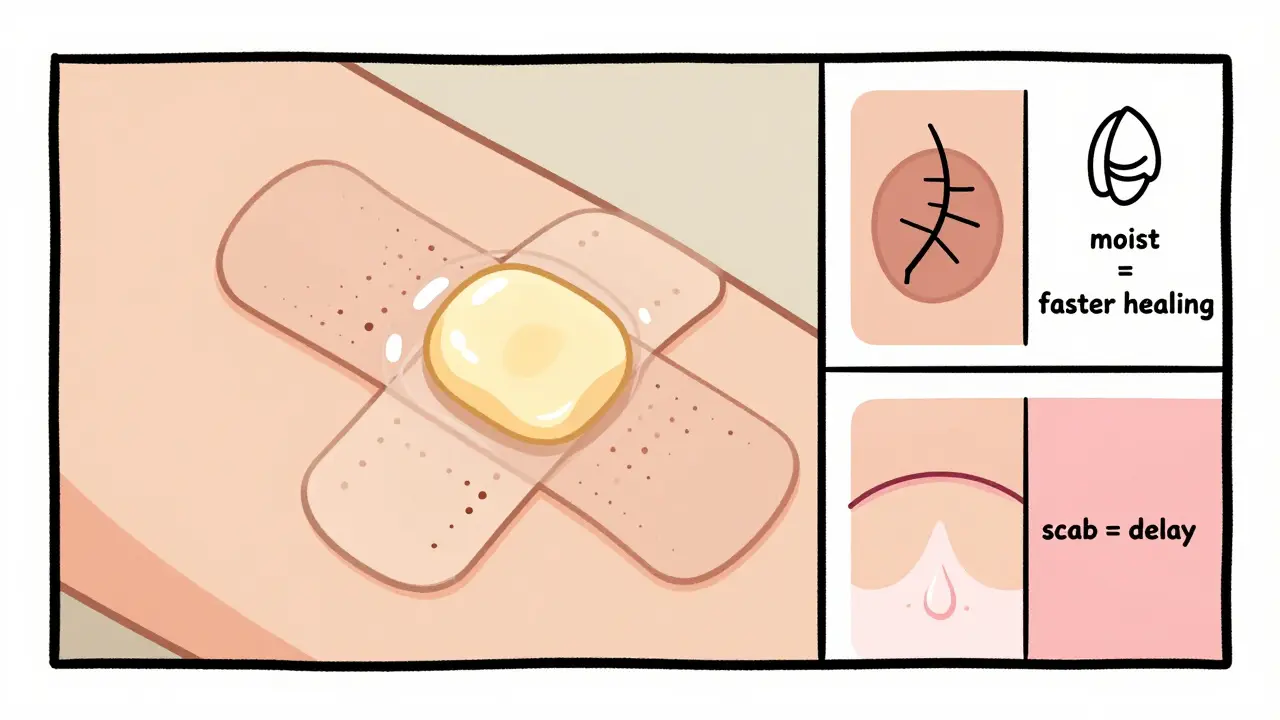
Step 2: Keep It Moist, Not Dry
Wounds heal faster when they’re moist, not dry. That’s why letting a scab form isn’t the best strategy. Scabs trap fluid and slow cell movement underneath. Instead, apply a thin layer of petroleum jelly or an antibiotic ointment like bacitracin. This creates a protective barrier that keeps the wound hydrated and stops bacteria from getting in.
Here’s the debate: do you need antibiotics? Most emergency rooms recommend bacitracin-it’s in 87% of wound care kits. But a 2021 study in JAMA Dermatology found that plain petroleum jelly works just as well for most minor wounds, with far fewer allergic reactions (3.2% vs. 8.7%). So if you’re not at high risk for infection, skip the ointment. Stick with jelly. It’s cheaper, gentler, and just as effective.
Step 3: Choose the Right Dressing
Dressings aren’t just bandages. They’re tools that control moisture, protect the wound, and support healing. Change them daily-or sooner if they get soaked. Pulling off a stuck dressing hurts and tears new skin. To avoid that, soak it gently with saline or water before peeling it off. Never tape a bandage completely around an arm or leg. That can cut off circulation and cause serious damage.
Match the dressing to the wound:
- Low drainage (dry or slightly moist): Use a hydrocolloid dressing. These stay on for days, seal out bacteria, and keep the area moist.
- High drainage (oozing): Use foam or alginate dressings. They soak up fluid without sticking.
- Deep or irregular wounds: Silicone sheets or non-adherent pads with gauze work best.
For burns, cool the area under running water for 10-15 minutes. Never use ice. Leave blisters alone-they’re nature’s bandage. Popping them raises infection risk by 35%.
Step 4: Prevent Scars Before They Start
Scars aren’t inevitable. With the right steps, you can cut their visibility by up to 60%. Start once the wound is closed and no longer oozing-usually around day 10 to 14.
Keep applying petroleum jelly or silicone gel daily. Silicone products are backed by strong evidence: studies show they reduce hypertrophic scars by 50-60%. Brands like Mederma or ScarAway are common, but even generic silicone sheets work. Wear them 12 hours a day for at least 8 weeks.
And don’t forget the sun. UV rays darken healing skin by up to 80%. Even a faint scar can turn into a dark, noticeable mark if exposed. Use SPF 30+ sunscreen on the area every day for at least 12 months. Hats and long sleeves help too.
Special Cases: Diabetic Wounds, Burns, and Pressure Sores
Not all wounds are the same. Some need extra care.
Diabetic wounds: People with diabetes heal slower and are more prone to infection. Even a small cut can turn into a serious problem. Check your feet daily. If a wound doesn’t improve in 2-3 days, see a doctor. Diabetic foot ulcers have a 40% higher complication rate than regular wounds.
Burns: Minor burns (first-degree, red and painful) respond well to cool water and moisturizer. Second-degree burns with blisters need medical attention. Never pop blisters. Cover loosely with sterile gauze.
Pressure sores: These happen when skin is under constant pressure-like from lying in bed too long. Prevention is key. Use cushions, shift position every 2 hours, and keep skin dry. The National Pressure Injury Advisory Panel recommends elevating heels off the bed and positioning at a 30-degree angle to reduce pressure by 65%.
When to Call a Doctor
Most wounds heal fine at home. But some signs mean you need help fast:
- Redness spreading more than an inch from the wound
- Pus or thick, yellow/green discharge
- Fever above 100.4°F (38°C)
- Wound doesn’t improve after 7 days
- Wound is deeper than 1/8 inch or longer than 1/4 inch
- Wound is on the face, hand, or near a joint
These aren’t just inconveniences. Redness spreading? That’s often cellulitis-a bacterial infection that can spread fast. Pus? Almost always infection. Don’t wait. Get checked.

What Else Helps Healing?
Wound healing isn’t just about what you put on the skin. Your whole body plays a part.
- Drink water. Dehydration slows healing by 25-30%. Aim for half a fluid ounce per pound of body weight daily. For a 150-pound person, that’s about 75 ounces-roughly 9 glasses.
- Eat protein. Your skin rebuilds with protein. Chicken, eggs, beans, tofu-all help.
- Avoid smoking. Nicotine cuts blood flow to skin. Smokers heal 50% slower than non-smokers.
These aren’t extras. They’re essentials. You can do everything right with dressings and cleaning, but if you’re dehydrated or smoking, your body can’t do its job.
What’s New in Wound Care?
The market for advanced wound care is growing fast-projected to hit $13 billion by 2027. New products include dressings with silver (reduces infection by 30%) and smart patches with sensors that detect pH changes, signaling infection before you even see it. But for most people? You don’t need them. Basic care-cleaning, moisture, protection-still works better than anything fancy.
Real progress isn’t in high-tech. It’s in consistency. People who follow simple protocols heal faster, with fewer complications, and less noticeable scars. It’s not magic. It’s just doing the basics right.
Can I use hydrogen peroxide to clean a wound?
No. Hydrogen peroxide damages healthy tissue and delays healing by up to 50%. It may kill bacteria, but it also kills the cells your body needs to repair the wound. Use cool running water and mild soap instead.
How often should I change a wound dressing?
Change it daily, or sooner if it’s soaked through. Leaving a wet dressing on too long lets bacteria grow. If you’re using a hydrocolloid dressing, it can stay on for several days-but check it daily. If it starts peeling or leaking, replace it.
Is it better to let a wound dry out or keep it moist?
Keep it moist. Dry wounds form scabs, which slow healing and increase scarring. Moist environments let skin cells move faster across the wound. Petroleum jelly or silicone gel helps maintain this moisture without sticking or irritating the skin.
Do I need antibiotic ointment for every cut?
Not usually. For minor cuts and scrapes, plain petroleum jelly works just as well and has fewer side effects. Antibiotic ointments are useful for higher-risk wounds-like those from dirty objects or in people with weakened immune systems. But for most people, they’re unnecessary and can cause skin irritation.
How long should I use sunscreen on a healing scar?
At least 12 months. UV exposure can darken a scar permanently, making it more noticeable. Even after the skin looks healed, the tissue underneath is still sensitive. Apply SPF 30+ daily, even on cloudy days. Covering the area with clothing or a hat helps too.
When should I go to the doctor for a wound?
Go if: redness spreads beyond 1 inch, you see pus, you have a fever, the wound isn’t improving after 7 days, it’s deeper than 1/8 inch, or it’s on your face, hand, or joint. These are signs of infection or serious damage. Don’t wait-early treatment prevents bigger problems.
Final Tip: Consistency Beats Complexity
You don’t need to buy expensive creams, fancy dressings, or follow 10-step routines. The most effective wound care is simple: clean with water, keep it moist, cover it right, protect it from the sun, and watch for warning signs. Do this every day, and your body will do the rest. Most scars aren’t from bad luck-they’re from skipped steps. Don’t skip yours.




February 21, 2026 AT 14:58
Just wanted to say this post saved my skin after I messed up a burn last summer. I used peroxide like everyone else-big mistake. Red, angry, took forever. Started following this guide? Healing cut in half. No scar. Seriously, do the water rinse and Vaseline. It’s dumb simple but it works.
Also, hydration is REAL. I started drinking more water and my cuts stopped getting crusty. Mind blown.